Acceptance of Vaccination Associated with Lower Social Media Use and Higher Trust in Government
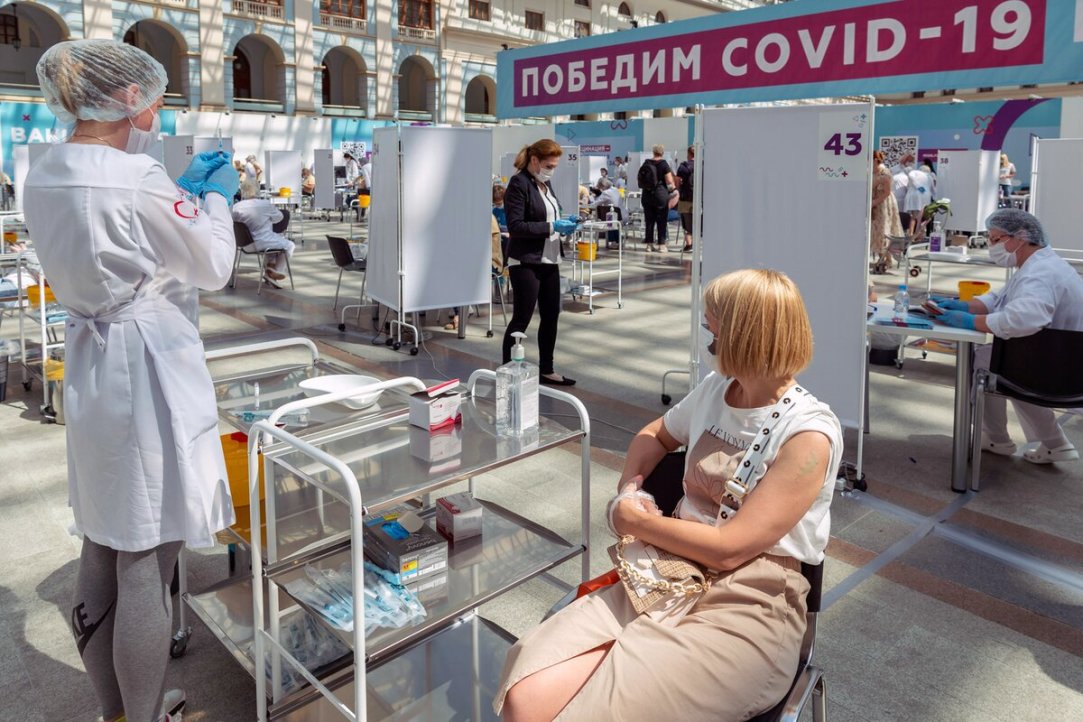
Vaccination is generally considered an essential tool for curbing the COVID-19 pandemic. Although Russia was one of the first countries to develop a vaccine against COVID-19 and launched an immunisation campaign in 2021, its vaccination rates remained low for a long time. By October 2021, only 36% of Russian adults were vaccinated, many of whom were compelled by their employers to do so. Having examined the factors contributing to low trust in vaccination among Russians, HSE economists suggest measures to improve vaccination uptake. The paper is published in Vaccine.
The paper uses data from the 29th wave of HSE's Russia Longitudinal Monitoring Survey (RLMS-HSE), conducted in the autumn of 2020. The survey respondents were asked, 'Are you planning to get vaccinated against COVID-19 once a vaccine becomes available?'.
No particular vaccine was mentioned, as all vaccine candidates were then at the trial stage. The answers, therefore, reflect the respondents' general attitudes towards vaccination. It was found that only 8% of respondents would ‘certainly’ get vaccinated, 36% would get a vaccine only if they were convinced of its safety and reliability, 44% did not intend to get vaccinated at all, and 13% were not sure. The responses reveal a high degree of resistance to vaccination even before any vaccine became available, and also a degree of ‘conditional acceptance’, as more than a third of respondents made their vaccination decision conditional on the future vaccine's quality.
This is the first paper in Russia to use multivariate econometric modelling to pinpoint the key determinants of COVID-19 vaccination attitudes on a sample of 8529 Russians aged 18 and older.
The advantage of RLMS-HSE is that it is not limited to standard socio-demographic data, but covers a wide range of individual characteristics, such as the use of social media, religiosity, and trust in government institutions. These characteristics, as well as the COVID-19 incidence rate in each surveyed region (measured as a 7-day moving average preceding the day of the survey), were included as independent variables in the regression model that revealed significant differences across four categories of respondents. While no differences in gender or income were observed, those who absolutely rejected vaccination included both younger and older respondents who self-rated their health as either 'very good' or 'very bad'.
Vaccine rejectors were also likely to have a lower level of education and a higher risk tolerance, and to live in Moscow or St Petersburg. Compared to those who would 'conditionally accept' a vaccine, rejectors reported higher levels of both neuroticism and agreeableness and had a higher proportion of those who never attended church as well as those who attended church at least once a month. They also reported less trust in government institutions and estimated their risk of contracting COVID-19 as low.
Those prepared to accept vaccination unconditionally reported the highest level of trust in government and rarely used social media. This finding may be significant, since social media served as an important source of information about COVID-19 vaccines, although they often spread anti-vax conspiracy rumours. Compared to 'conditional accepters', rejectors tend to be more friendly but less extroverted, and slightly more likely to be atheists. People who have already had COVID-19 are also more likely to be found in the 'rejector' group.
The researchers conclude that attitudes towards vaccination are shaped by a variety of socio-economic and personality factors, including one's risk appetite and trust in government.
The authors also suggest that vaccination-promoting policies need to take into account the observed distinctions across these four groups.

Yana Roshchina, Leading Research Fellow of the HSE Institute for Social Policy and Senior Research Fellow of the HSE Laboratory for Studies in Economic Sociology
'Perhaps hard data on vaccine effectiveness and safety could help convince those who hesitate, while those who reject vaccination altogether need a different approach. They may be generally lacking vaccine literacy; therefore, educating them about achievements in science and medicine could improve vaccination uptake in this group.'
Yana Roshchina
Senior Research Fellow, Laboratory for Studies in Economic Sociology

